April MITE Hot Topic – PDSA Cycles for Continuous Improvement
Author: Hilary Perrey, MHA, LSSBB
Improvement Specialist II
Maine Medical Center Performance Improvement
Learning Objectives:
- Describe what PDSA cycles are and how we use them in continuous improvement.
- Explain how to conduct PDSA cycles.
- Illustrate a helpful PDSA cycle template.
Have you ever heard a beautiful symphony orchestra and wondered how they achieved such musical perfection? How did a particular surgeon gain advanced technical skill in his or her profession? Plan – Do – Study – Act (PDSA) cycles are a four-step model for change and can be used in achieving continuous improvement – from a symphony to the operating room.
Walter Shewhart, a statistician at Bell Telephone Laboratories, developed the Shewhart Cycle in the 1920’s.1 The Shewhart Cycle is best known as the Plan – Do – Check – Act (PDCA) cycle. In 1993, W. Edwards Deming adapted the PDCA cycle as the Plan – Do – Study – Act (PDSA) cycle.2 Just as a circle has no end, the PDSA cycle can be repeated for continuous improvement. The PDSA cycle is also known as the Deming Cycle or the Deming Wheel.1
The MaineHealth branded PDSA template (figure 1) can be used in continuous improvement and quality improvement efforts. The following example illustrates a PDSA in action from the Oncology Service Line’s Multidisciplinary Thoracic Review (MATRIx) Program. The MATRIx Program was the FY19 Oncology Service Line’s Clinical Transformation Project and subsequently its FY20 Maine Medical Partners quality improvement initiative. The goal of the MATRIx project was to decrease time to surgery and time to various clinical endpoints for patients on different referral and treatment pathways.
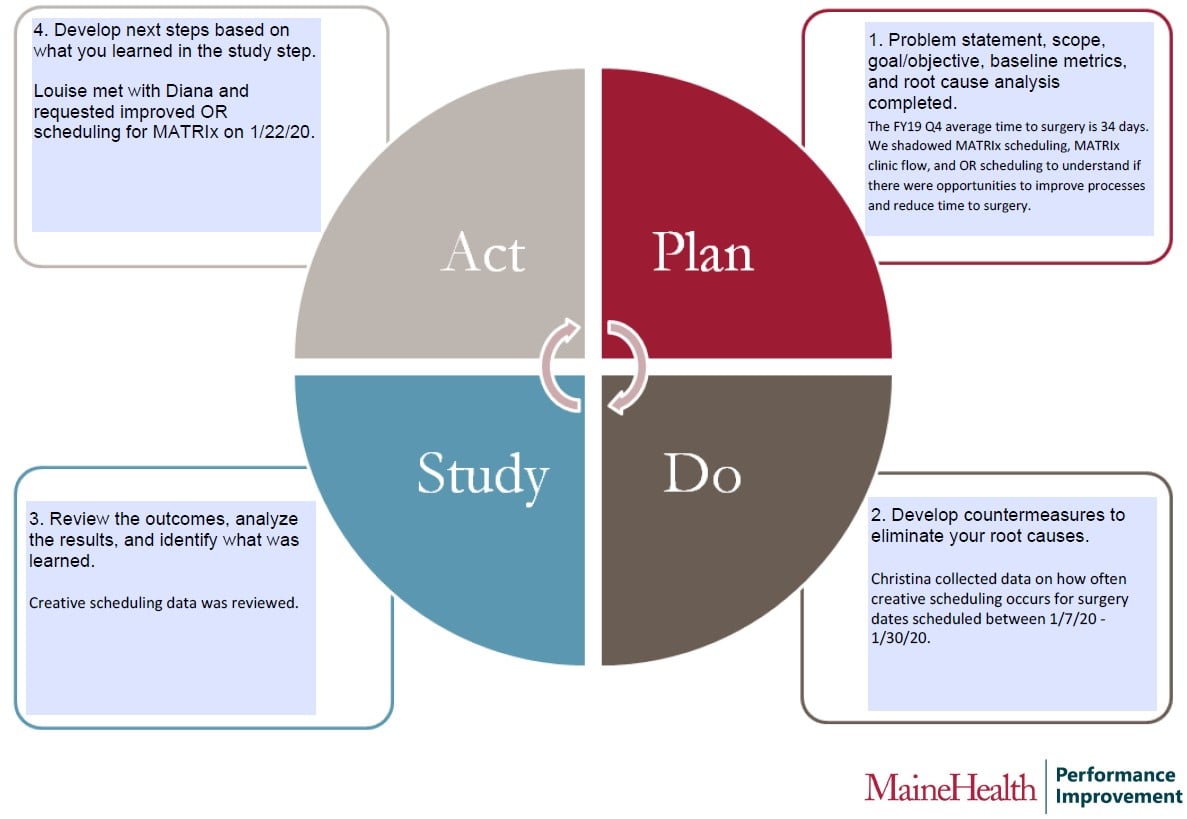
The MATRIx team sought to increase efficiencies in OR scheduling as a means to decrease time to surgery for patients with suspicious lung nodules (figure 2). In the Plan phase, the baseline average time to surgery in FY19 Q4 was 34 days. Our team shadowed MATRIx scheduling, MATRIx clinic flow, and OR scheduling to understand if there were opportunities to improve processes and reduce time to surgery. In the Do phase, the clinic’s Office Manager collected data on how often creative scheduling occurs for surgery dates scheduled between 1/7/20 – 1/30/20 to understand how frequently scheduling workarounds are needed. In the Study phase, creative scheduling data was reviewed. In the Act phase, the Senior Director of Oncology Services met with the Director of Perioperative Services and requested improved OR scheduling for the MATRIx Program. Subsequently, the OR and MATRIx team collaborated to prioritize thoracic surgeries for cancer patients. The Medical Director of Thoracic Surgery advocated for an increase from one to two dedicated surgical teams so each thoracic surgeon can operate with its own team, cycling back into Plan. The thoracic surgeons trained an additional surgical nurse and technician and now have two dedicated thoracic surgery teams which may improve scheduling, time to surgery, and increase surgical volume (more Do, Study, and Act). This PDSA cycle demonstrates how incremental improvement can be achieved and how one PDSA cycle leads to another. This is the path of continuous improvement.
Figure 1. MaineHealth PDSA template
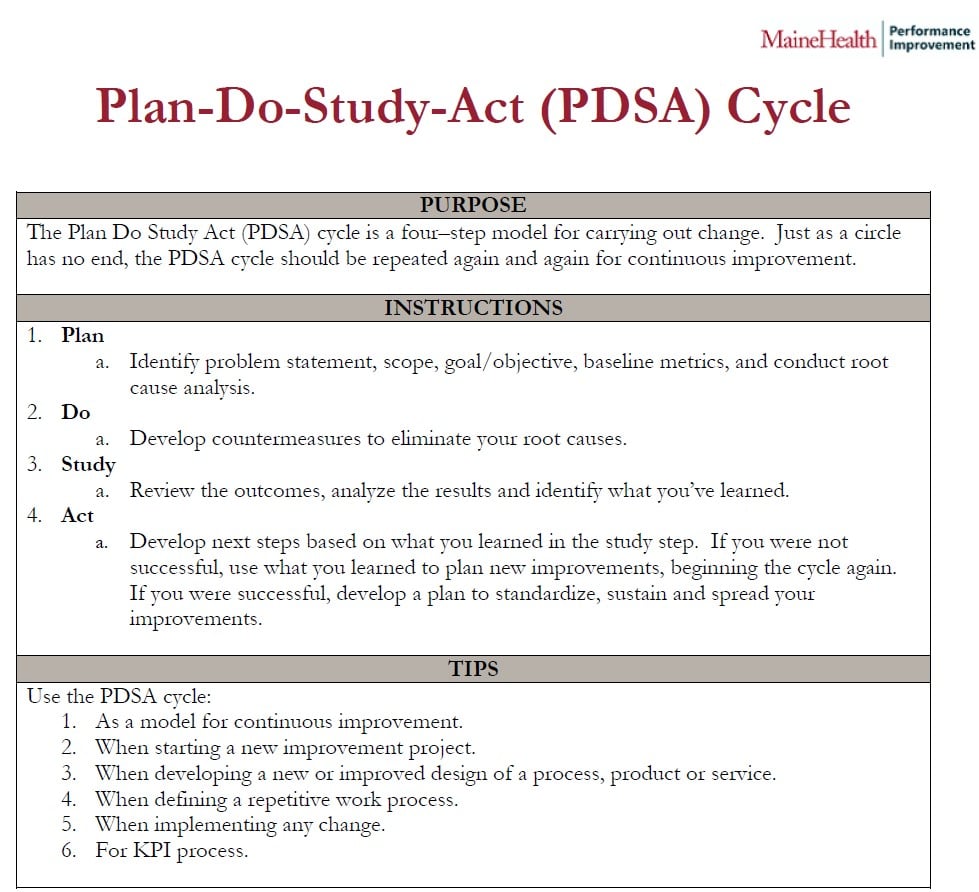

The PDSA cycle template and other MaineHealth Performance Improvement tools can be accessed via SharePoint at https://home.mainehealth.org/2/MMC/CenterforPerformanceImprovement/SitePages/AllTools.aspx.
References:
- Luc R. Pelletier, Christy L. Beaudin. HQ Solutions Resource for the Healthcare Quality Professional, Fourth Edition, 2018. National Association for Healthcare Quality.
- Ronald Moen. Foundation and History of the PDSA Cycle. Microsoft Word – PDSA_History._16th_Deming_Research_Seminar_Feb._2010.Moen.docx
Want to earn CE Credits? Click here!
Download PDF